A Guide To Skin Infections
What are the differences between bacterial, viral and fungal infections?
These are caused by different types of organisms and they require treatment with different medications. For example, antibiotics will work only for bacterial infections and not for viral or fungal infections. It is therefore important to recognise the different types of infections and have them diagnosed accurately before treatment.
What are some common bacterial infections?
Folliculitis is an infection of the hair follicles (hair roots). It presents as a red ‘pimple’ around a hair follicle. If folliculitis is not controlled and spreads to involve deeper areas of the skin, a boil or abscess develops. This contain pus and is often painful. Fever can also develop.
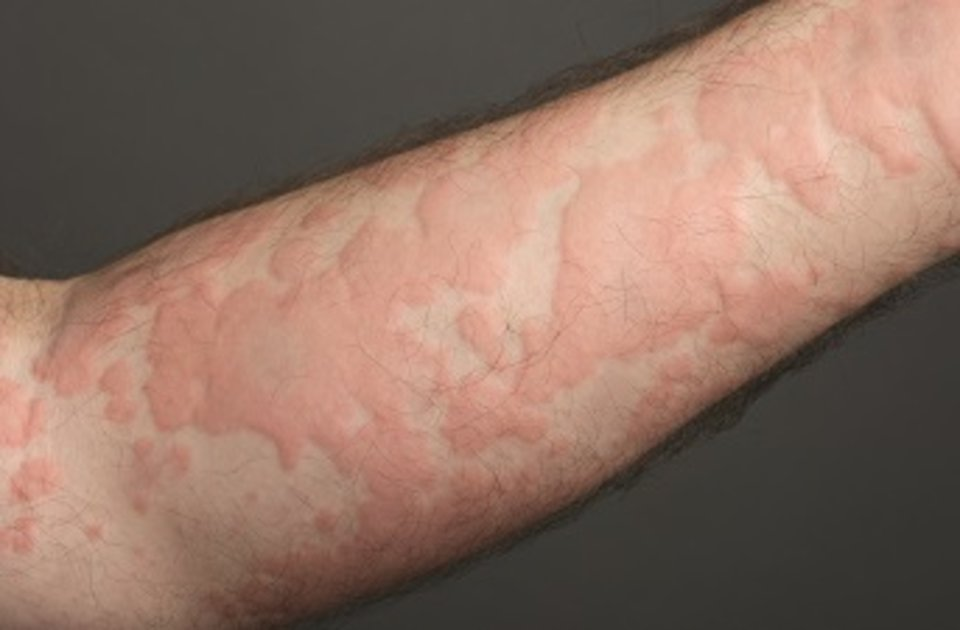
Cellulitis is a serious type of skin infection which affects the deeper layers of the skin. It can occur though a break in the skin e.g. cuts, insect bites. Patients with underlying skin disease (e.g. eczema) or diabetes are more prone to developing cellulitis. Cellulitis usually involves one part of the body, such as the leg or arm. The affected area ¡s swollen, often feels warm, is sore to touch and appears red. A fever may also develop.
Impetigo is another type of bacterial skin infection that usually affects children. It is more commonly seen in patients with underlying skin disease (e.g. eczema). Blisters can develop and these break down to leave yellow crusts. There is a tendency for the infection to occur around the nose, mouth and legs. Impetigo can be contagious and spread from one child to another through close contact.
How are bacterial infections treated?
Your doctor will usually prescribe oral antibiotics. If the infection is localized to an area of the skin, an antibiotic cream may be prescribed instead. It is important to complete the course of oral antibiotics, even if you start feeling better after one or two days. When treating large boils, a procedure to drain the trapped pus may be necessary. Serious bacterial infections like cellulitis sometimes require admission to hospital for antibiotics though a needle into the vein. If you are allergic to any antibiotics, you must remember to inform your doctor. Some commonly used antibiotics indude penicillin, amoxicillin, cloxacillin, cephalexin and erythromycin.
What are the dangers of not receiving treatment?
Sometimes the infection can spread beyond the original site and make the patient extremely ill, and occasionally, this can be life threatening. In children, elderly patients, and patients suffering from diseases such as diabetes or cancer, bacterial infections should be treated as soon as possible to reduce the chance of serious complications developing.
What are some common fungal skin infections?
Tinea versicolor
This is known commonly as ‘white spots’ or ‘panau’ (in Malay) or ‘sweat spots’. It is caused by a yeast organism that commonly lives on the skin of humans. It tends to affect adolescents and young adults. Poor personal hygiene may increase the change of infection. Sometimes, the spots appear pink or light-brown. It may be itchy especially after sweating. The commonly affected areas are the chest and the back.
Is the colour change permanent?
No. Usually the skin will slowly return to its normal colour after treatment. However, the white areas may remain for a few months after treatment, and this is not a sign that the treatment has not worked.
Why do I keep getting ‘white spots’?
The infection can recur, especially in people who are active physically. This means that you can become infected with the yeast organisms again. Re-treatment would be necessary.
Ringworm
The term ringworm refers to a common type of fungal infection of the skin. The affected area tends to take on a ring-like configuration hence the term, ringworm. Ringworm tends to affect moist areas such as the groins, inner thighs, feet and buttocks. However, any part of the body can be affected.
What does ringworm look like?
Affected areas appear as a dark area surrounded by a ring of red, scaly bumps. Itch is common.
‘Hong Kong foot’ or ‘Athlete’s foot’?
This is a fungal infection of the feet. The web spaces between the toes are often affected. The soles appear scaly. Less commonly, small water bubbles or spots containing pus appear. The toenails can also be affected and look unhealthy, with a yellowish discolouration and thickening seen under the nails. Scrapings of the skin scales and clippings of the affected nails can be sent to the laboratory for tests to confirm presence of fungal infection.
Are fungal infections contagious?
Yes, fungal infections can occur because of frequent, close contact with someone who is already infected. It is more easily spread in areas of the skin which are moist, for example the groin or toewebs. Sometimes people can get infected from walking barefooted in wet areas such as swimming pool floors.
Can fungal infections be cured?
Yes. Your doctor will prescribe an anti-fungal cream or lotion, and sometimes, tablets. It is important for you to continue to use the cream for another 1-2 weeks after the rash has resolved. This is to kill any remaining fungal cells that may not be visible to the naked eye. Tinea versicolor (white spots) can be treated with shampoos containing anti-yeast medications and topical anti-fungal creams or lotions.
How can I prevent fungal infections?
Keep your skin dry and practice good personal hygiene. Wash off sweat with mild soap and water and keep skin folds dry. Use of powder helps. Avoid walking barefooted on moist areas like swimming pools, public toilets and common showers. Try to change your footwear and alternate between two pairs of shoes so that the shoes get a chance to dry out. Avoid sharing items such as towels. Weight reduction in overweight individuals also helps.
I have fungal infection of my nails. Can this be cured?
Fungal nail infections can be treated but it often requires prolonged treatment. Anti-fungal tablets have to be prescribed by doctors. Certain tablets (like griseofulvin) may have to be taken continuously for up to 18 months; there are other alternatives where a patient takes medication for 2 to 3 months or one week out of every month for 3-4 months (pulse therapy). You should not take these oral medications if you are pregnant or planning a pregnancy. Anti-fungal nail lacquers can also be used either alone or in combination with tablets. Your doctor will advise you on the best options.
After treatment for fungal nail infections, my nails still look abnormal. Why is this so?
Eradication of the fungus does not guarantee that the appearance of the nails will return to normal. Furthermore, nails grow very slowly, so the affected nail takes a long lime to be replaced by normal looking nails. Another possibility is that there may be other causes for the abnormal appearance of your nails, like psoriasis. You should see your dermatologist for advice.
What are some common viral skin infections?
Viral warts (verruca), molluscum contagiosum (water warts), herpes zoster (shingles), herpes simplex infections are common viral infections of the skin. Viruses can cause infections of the skin directly. These include viral warts, herpes zoster (‘shingles’) and molluscum contagiosum. In other situations, a viral infection such as an upper respiratory tract infection may cause a rash to appear. This is called an ‘exanthem’ or viral rash.. It is a kind of reactionary rash and usually fades after a few days or weeks.
Viral warts
What do they look like?
Viral warts usually appear as small flesh-coloured lumps. They can have a rough surface, or appear quite flat. When they affect the soles of the feet, they are often mistaken for ‘corns’.
Do they cause itching or pain?
Warts are usually not itchy. Warts on the soles (plantar warts) can become thick and give rise to pain on walking.
How are warts treated?
Cryotherapy with liquid nitrogen is a common form of treatment for warts. The treatment is perform once every 1-2 weeks in the clinic. It is like applying ‘dry ice’ to the wart to destroy it. It does cause mild pain but this is usually tolerated quite well by most patients. Sometimes, a blister forms over the treated area. You should let the area heal by itself. Other treatment methods include applying acidic solutions, commonly containing salicylic acid and/or lactic acid, electro-surgery or using a laser. It is important to note that warts may recur even after adequate treatment, regardless of the type of treatment.
Why can’t I be treated with a laser from the beginning?
Laser treatment is usually reserved for warts which have not responded to simpler methods of treatment, as treatment is painful and expensive. Most common warts can be treated with cryotherapy with liquid nitrogen treatment.
Can warts spread to other people?
Yes. Warts can be passed from one person to another by direct contact.
Molluscum contagiosum
Molluscum contagiosum is caused by a virus different from that which causes viral warts. The infection usually occurs in children. They appear as small whitish or skin-coloured, shiny, dome-shaped lumps, sometimes with a dimple or small depression in the centre. Molluscum can spread from one area of the body to another through scratching. They can also spread from person to person.
Is it dangerous?
Molluscum are not dangerous. They can sometimes disappear on their own without treatment but this may take months. When the surrounding skin becomes red, itchy and irritated, this may herald spontaneous resolution in a few weeks or months.
How are molluscum treated?
There are several ways to treat molluscum. The lesions can be pricked with a sterile needle and extracted (this procedure is like extracting a whitehead in a patient with acne). An acidic solution or creams like imiquimod or tretinoin can also be applied to treat the lesions. Liquid nitrogen or electro-surgery may also be used, but may cause significant pain. A numbing gel can first be applied an hour before the procedure and this would be helpful when treating children.
Can’t I take a tablet to make the warts or molluscum disappear?
At the moment, there are no effective oral medications which are effective for the treatment of molluscum.
Shingles / Zoster
What is it?
This is an infection caused by the same virus that causes chickenpox. It represents a reactivation of the chickenpox virus. It presents as painful blisters occurring on one side or segment of the body. It is often referred to as ‘snake’ by the Chinese.
It is believed that if the ‘snake’ forms a complete circle around the body, I will perish. Is this true?
No. The condition is usually not life-threatening. However, if it occurs in a patient with a very weak immune system (e.g. a cancer patient on chemotherapy), it can be fatal.
Is there a tablet available to treat shingles?
Yes. Anti-viral medications (e.g. acyclovir, valaciclovir) is effective in reducing the severity and duration of shingles if it is taken early, i.e. within the first 3 days of appearance of the skin eruption.
How long does it take to recover?
It usually takes 10 to 14 days for the area to heal completely. You must keep the area clean to prevent secondary bacterial infection. Compresses to the area with saline water or potassium permanganate are soothing and will dry up the oozy areas. Sometimes an antibiotic cream can be applied to the areas with eroded skin.
I heard that the pain can continue even though the skin eruption has healed. Is this true?
Yes. Unfortunately, some people with shingles may suffer from prolonged pain even after the skin lesions have resolved. This is more common in the elderly and can last for months. The pain can be burning in nature, poking or sharp. Medications (e.g. NSAIDS, gabapentin) may reduce the severity and duration of the pain.
Infestations
Scabies
This is an infestation of the skin by a tiny mite, known as Sarcoptes scabeii. It is highly contagious and passed from person to person through close body contact. Patients present with a rash consisting of intensely itchy red spots on the insides of the arms, armpit folds, wrists, finger and toe webs, around the belly button, groins and the genitals. The rash usually develops few weeks after contact with an infected person. The diagnosis is usually made by observing the typical rash. Sometimes it is possible to find the mite buried in the skin by scraping the scaly burrows found on the skin surface and looking through a microscope.
Treatment is with application of lotions/creams containing benzyl benzoate, malathion or permethrin. It is imperative that family members and close contacts are treated at the same time regardless of whether they suffer from any symptoms.
Lice
There are 3 types of louse — head, body and pubic lice.
- Head lice: These commonly affect children. Their nits or eggs can be seen stuck on the hair shafts. If left untreated, the scalp will turn red and itchy. Spread is through close contact. The eggs remain alive on brushed-out hair and it is therefore important not to share combs.
- Body lice: This is not common. The lice feed on the skin and live in the seams of clothing.
- Pubic lice: The infected individual experiences intense itch on and around the genitals and often notices the lice crawling amongst the pubic hair. Pubic lice are usually spread through intimate contact.
Treatment for lice usually consists of lotions containing malathion or permethrine are effective in clearing the infestation. Classmates of affected children should be checked for hair lice.