Psoriasis: Causes, Types and Treatment
What is psoriasis?
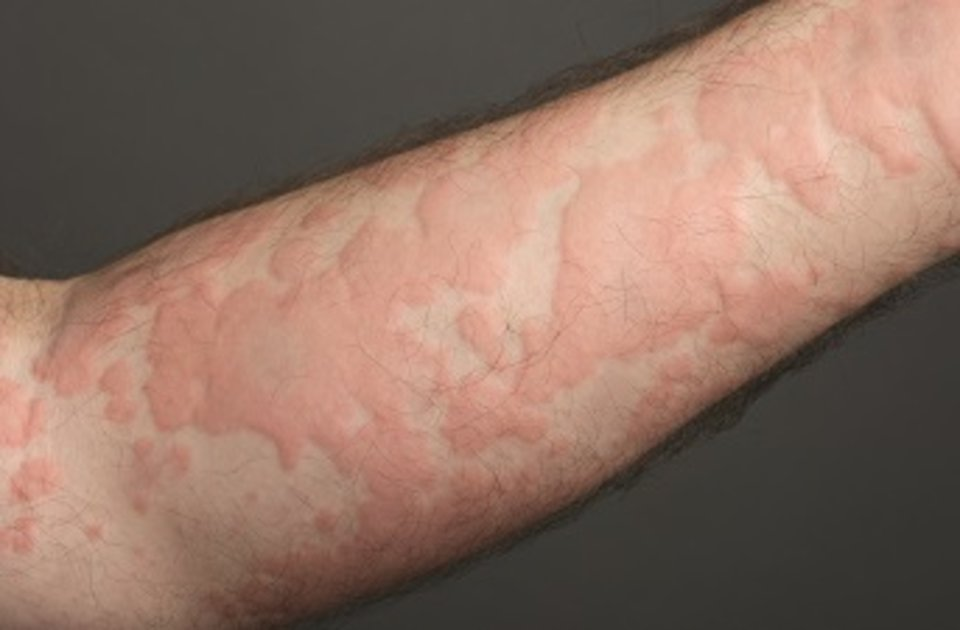
Psoriasis (pronounced without sounding the ‘p’) is a chronic, non-contagious skin condition whereby the skin cells multiply and are replaced too quickly. It is also accompanied by some inflammation. As such, the condition appears as red scaly patches.
What causes psoriasis?
No one really knows what causes psoriasis. There is a family pattern in one third of cases, and it is accepted that heredity plays a part. It is believed that multifactorial inheritance is involved in psoriasis. Certain environmental factors may trigger off psoriasis in persons who are predisposed genetically.
What happens in psoriasis?
There is abnormal cell growth in the skin of susceptible individuals. The turnover of normal skin cells takes place in about 28 days. In psoriasis, skin cells multiply more quickly than usual and move to the top layer of the skin in only 3 to 7 days.
As such the excessive dead skin cells heap up to form the thick white scales that we see on the red elevated patches of psoriasis.
Who gets psoriasis?
Both men and women can be affected by psoriasis equally. It affects about 0.5% to 2.0% of the population. It can also appear at any age, but mostly between the ages of 15 and 35. In Singapore, it is more common among the Indians compared to the other races.
Can diet affect psoriasis?
Although some patients claim that certain foods affect their psoriasis, this has not been confirmed by scientific studies. It is wise to keep to a balanced diet and keep yourself healthy.
Can I catch psoriasis from another affected person?
Psoriasis is not contagious and cannot be spread through touching, eating together or swimming in the same pool.
What can worsen psoriasis?
Mental stress often makes psoriasis worse. Any form of trauma to the skin can also make it worse. Skin injury e.g. cuts, burns, rubbing and scratching often lead to a worsening of psoriasis over the areas injured. Drug reactions and infections can also aggravate psoriasis.
Is there a cure for psoriasis?
Unfortunately, there is no one medication that can truly cure psoriasis, but there are good and effective treatments available that can control the condition or clear the patches. The skin may remain clear for a few weeks to severaly ears.
How is psoriasis diagnosed?
It is usually diagnosed by its typical appearance. In unclear cases, a biopsy may be helpful in establishing the diagnosis.
What does psoriasis look like?
There are various forms of psoriasis and severity is variable.
Plaque psoriasis
The most common type is plaque psoriasis. It appears as red elevated patches covered by silvery/whitish scales. Lesions often appear in a symmetrical manner i.e. they appear on the same places on both sides of the body. Areas often affected are the scalp, elbows, knees, arms, legs, ears and the lower back.
On the scalp, psoriasis may appear like bad dandruff when mild; the condition may develop into thick, scaly patches when severe.
Guttate psoriasis
Guttate psoriasis is more commonly seen in children and young adults. It appears as small red elevated spots, like ‘raindrops’ on the trunk and limbs. It can appear suddenly and may be triggered by a streptococcal throat infection, a common cold, chickenpox or immunizations.
Sometimes, guttate psoriasis may reappear with successive attacks of sore throat.
Pustular Psoriasis
Sometimes small pustules (small pockets of pus) may be present on the lesions making them look ‘infected’. This is called pustular psoriasis. It may be localized to certain parts of the body, or it may be generalized. In the generalized type, the patient can be quite ill with a high fever. Generalized pustular psoriasis can be provoked by the withdrawal of steroid tablets.
Erythrodermic psoriasis (erythroderma means red skin)
In this form of psoriasis, the skin appears as a diffuse redness and scaling.
Most affected individuals start by having what looks like bad, persistent dandruff for some time. Subsequently, scaly patches may appear on the body and the face.
Others
The nails may be affected and show small pits or appear lusterless, deformed and thickened in severe cases. Joint pains may also develop in 5 to 10% of cases. This is called psoriatic arthritis.
How is psoriasis treated?
Psoriasis can be treated in several ways depending on the type, the extent and areas involved. Once the psoriasis is cleared, the treatment is generally discontinued and only restarted when the psoriasis returns. There are various methods of treating psoriasis: creams or topical treatment, ultraviolet light, tablets (systemic drugs) and biological drugs.
TOPICAL TREATMENT
Topical treatment is used for mild to moderate psoriasis. These include cortisone creams (steroids), coal tar, dithranol, calcipotriol and moisturizers. These can be used alone, or in conjunction with other treatments.
What are steroids?
Steroids commonly known as cortisone are used to treat inflammatory conditions.
In psoriasis, it is usually used as creams, ointments and scalp lotions. Generally, for psoriasis, moderately potent topical steroids are used. Steroid tablets and injections are not used in psoriasis except for very special situations. The use of steroids requires a doctor’s prescription and supervision.
Are there any side effects from using steroids?
Yes, if it is not used carefully and under doctors’ supervision.
The following changes may develop following long-term use of very potent steroid creams: thinning of the skin, stretch marks, or easy bruising. Strong steroids on the face cause persistent redness and pimples. Most of these side effects resolve when steroid treatment is discontinued, but some like stretch marks can be very persistent. Psoriasis can sometimes become worse when the daily use of potent topical steroids is suddenly discontinued. This is called the ‘rebound phenomenon’.
Systemic steroids, i.e. steroids given as tablets or through injections, are not used in psoriasis except for very special situations because of the potentially serious side effects. When systemic steroids are discontinued, the ‘rebound phenomenon’ often occurs. Limited extent psoriasis may become generalized or pustular psoriasis may develop.
What is coal tar?
Tar is derived from crude coal tar and is made into creams, ointments and shampoos. Tar can suppress division of the cells in the skin and help to keep psoriasis under control. It can be used in combination with other treatment methods. Disadvantages: tar smells and stains clothing and bed linens. The onset of improvement is often slow.
What is dithranol?
Dithranol or anthralin is a synthetic compound that is effective in clearing mild and moderately severe forms of psoriasis. It also works by slowing down the division of cells in the skin. It is available in creams or ointments of various strengths. It is to be left on the affected area for 30 minutes, then washed off in order to reduce irritation of the skin. This is not commonly used nowadays due to the irritation potential.
What is calcipotriol?
Calcipotriol is a compound that is derived from vitamin D. It has been shown to slow down the increased multiplication of cells, normalize cell maturation and the abnormal immune response that occurs in psoriasis. Calcipotriol has been found to be as effective as topical steroids, and more effective than tar or dithranol.
Calcipotriol is available in creams and ointments and also as a scalp application. Calcipotriol may cause mild skin irritation and it is not advisable to be used on the face.
Other topical preparations
An important part of treatment for psoriasis is the use of moisturizers or emollients.
Lubrication helps to soothe the skin, making it less itchy and uncomfortable. It also helps other applied medications work better. Lubrication with moisturizers after bath will help to prevent dryness of the skin.
ULTRAVIOLET LIGHT TREATMENT
What is it and how is it used?
Ultraviolet light, UVB and UVA, are both present naturally in sunlight and are used to treat psoriasis. Artificial light sources emitting either UVA or UVB are utilized.
UVA light is used in combination with a medication called Psoralen and the treatment is called PUVA (Psoralen + UVA). Ultraviolet light treatment is considered for patients who have extensive psoriasis or not responsive to topical treatment.
UVB treatment
UVB is the light that is most commonly used. It helps in 70.8% of patients with psoriasis. Treatment is usually carried out in a cabinet equipped with light tubes that emit UVB so the whole body can be treated in one exposure. Treatment is usually carried out 2 to 3 times weekly and the dose of ultraviolet radiation is gradually increased. Exposure to this light is usually short, i.e. a few minutes. Side effects from this treatment are few. An acute sunburn can sometimes occur when an overdose is administered.
Recent studies have shown that a particular portion of UVB at wavelength 313nm is more effective in clearing psoriasis than the entire UVB segment of ultraviolet light. Narrow band UVB light tubes which emit a narrow band of light at 313+/-3nm are now replacing the conventional broad band UVB lamps in the treatment of psoriasis.
PUVA treatment
UVA alone is not very useful in treating psoriasis. It is used in combination with a medication called psoralen. This treatment is called PUVA (Psoralen + UVA). A patient on PUVA takes the medication about 2 hours before exposure to UVA light. UVA is delivered in a light chamber fitted with light tubes that emit UVA light. Psoralen makes the skin much more sensitive to UVA and it also enhances the ability of UVA to reduce cell multiplication and thereby improves psoriasis.
PUVA is more effective than UVB in the clearing of psoriasis.
The most common short-term side effects of PUVA are nausea from taking the psoralen tablets and a burn resulting in redness and itch. Deep tanning of the skin develops quickly with PUVA therapy and tends to be long lasting. There is a risk of development of skin cancers if PUVA is used on a long term basis.
ORAL MEDICATIONS FOR PSORIASIS
Oral medication is an option for patients who have severe or extensive psoriasis but unable to have phototherapy or fail to respond to phototherapy. The commonly used tablets are methotrexate and cyclosporin. Other medications that are sometimes used include acitretin.
What is methotrexate?
Methotrexate is a highly potent medication which slows down the rapid multiplication of cells seen in psoriasis and helps restore the skin to a normal state. It is taken in small doses once a week. It is best used for extensive psoriasis, physically disabling psoriasis, psoriasis in the elderly and psoriasis affecting the joints.
Methotrexate is effective in more than 70% of patients; it is a convenient form of treatment and the results are usually predictable.
What are the side effects of methotrexate?
Methotrexate can potentially damage the liver especially if it is taken on a long term basis and it can also suppress the bone marrow. It is metabolized in the liver and excreted by the kidneys. As such, before commencing treatment with methotrexate, it is necessary to do blood tests to check on the blood cells count, liver function and kidney function. Periodic tests are also done while the patient is taking methotrexate. Methotrexate is not suitable for patients who drink regularly as there is a risk of liver damage. It is also not suitable for men and women planning to start a family.
Other common side effects of methotrexate are nausea, vomiting, headache and dizziness while taking the medication.
What is cyclosporin?
Cyclosporin is a drug which suppresses immune responses. It has been found to be useful in psoriasis in low doses. It is indicated for patients with severe psoriasis not responsive to conventional treatment mentioned above, and in those whose psoriasis is physically and socially disabling.
Cyclosporin should not be used in patients with kidney disease, uncontrolled high blood pressure, history of cancer, infection, or who are pregnant or breast feeding.
Side effects include effects on the kidneys and hypertension. As it suppresses immune responses, infections can be made worse. Patients on cyclosporin should be monitored carefully by doing regular blood tests.
What is acitretin and what are the side effects?
Acitretin belongs to a group of medications called retinoids which are derived from vitamin A. It acts by normalizing the increased rate of multiplication and abnormal maturation of skin cells which occurs in psoriasis. It also has anti-inflammatory effects. Used on its own, it is effective in severe erythrodermic psoriasis and pustular psoriasis. For chronic plaque type psoriasis, excellent results can be achieved when it is used in combination with PUVA or UVB.
Side effects of the drug include dryness of the skin, lining of the nostrils, the mouth and lips. Rarely, it can affect the liver, and it can also cause a rise in the blood lipids. If women while on acitretin get pregnant, there is a risk of congenital defects in the baby. It is therefore not recommended for women who intend to get pregnant.
BIOLOGIC DRUGS
What are biologic drugs?
Biologic drugs (or biologics in short), are newer medications used to treat psoriasis by targeting specific molecules of the immune system that are driving the psoriasis on. These molecules are over-expressed (i.e. over-activated) in patients with psoriasis.
How effective are biologics and how are these drugs administered?
As biologic agents are considered ‘smart’ drugs, they are very effective in clearing the psoriasis as long as the patient is on the drug. It does not confer a cure for psoriasis. Most of the biologic drugs are administered by injections into the skin (subcutaneously) or into the vein (intravenously). The dosing schedule for these drugs vary from once a week to once every 3 months, depending on the type of drug injected.
What are the side effects of this drug?
Generally, these biologic agents are quite safe if given in the right context and proper monitoring is done. Screening blood tests to make sure that the blood counts, liver and kidney function are normal is compulsory. Any underlying infections, e.g. hepatitis B and C, HIV as well as TB (tuberculosis) should be tested for and treated if a patient is considering biologics. The risk of TB reactivation with some of the biologic agents requires the doctor to test for the presence of latent TB prior to starting these drugs. As biologic drugs are relatively new in the market, the long term (i.e. 20 years or more) side effects are not known.
What can be done about psoriasis of the joints?
Up to one-third of patients with psoriasis have psoriatic arthritis. It can affect both the small joints of the fingers and toes, or the large joints of the limbs and spine. like other forms of arthritis, affected patients experience stiffness, aches and pains. The pain and swelling can be treated with anti-inflammatory medications and if the arthritis is progressive, methotrexate or certain biologics should be considered.